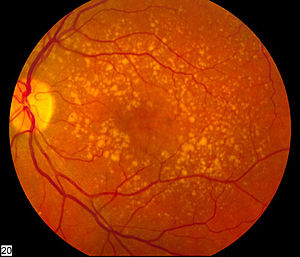

Age-related Macular Degeneration (AMD)
Age-related macular degeneration (AMD) is a serious condition of the eye and responsible for nearly half of the cases of blindness above the age of 60. AMD ranks third, globally, as a cause of blindness after cataract and glaucoma. An estimated 11 million people were affected by AMD in the United States alone, and 170 million worldwide in 2016 [1].
AMD develops on the macula, the central part of retina, where light-sensitive cells are organised with the purpose to capture the image formed inside the eye and pass it dorsally via optic nerves to the brain. The retina, like all body parts, goes through natural wear and tear process with aging. This process manifests itself as toxic yellowish-brown cell debris and deposits called drusens. Gradually, the retina fails to regenerate, reconstitute and renew the parts that are affected by accumulating drusens, which leads to geographical atrophy (cell death) or GA.
Early stage of AMD, also known as “dry” AMD is characterised with drusens and GA and is associated with varying degrees of loss in visual acuity. In the advanced stage, leaky capillaries may form in the mid-layer of the eye, known as choroid layer. Leaking blood and fluid from these capillaries ensues more damage to the macula. This stage is known as “wet” AMD, which, although accounting for a small portion of the AMD cases, is a more serious concern, because it is the cause of 80 to 90% of all legal cases of blindness associated with the disease.
Direct injections of medicine into the eyeball (intravitreal) is the current treatment modality for wet AMD. Type of medications known as anti-angiogenic drugs (anti-VEGF drugs, block vascular endothelial growth factor activity, and cease the formation of new leaky capillaries) may slow down the progression of the disease and enable to partially restore vision.
Clinical imaging techniques have seen expanding applications in the development of effective therapies and tackling the disease, mainly due to the growing number of morphological signs that can assist the early prediction of wet AMD before it causes irreparable damage.
Colour Fundus Photography (CFP) has been a mainstay method for detecting drusens and other morphological changes, by using broad spectrum illumination device. Low contrast and low sensitivity in detecting key biomarkers of AMD, compared to other imaging devices, limits the use CFP.
Fundus Autofluorescence (FAF) imaging, utilizing blue light excitation to acquire retinal images provides sharp contrast and image resolution in detection of atrophic areas on the macula. The pigment retinal epithelium (RPE) and lipofuscin, the “wear-and-tear” pigment of yellow brown, are severely lost in atrophic areas and FAF imaging can provide a strong correlation between structure and function; and intact and degenerating retinal tissue.
While CFP and FAF imaging are clinically practical for grading GA and detecting drusen morphology, both provide limited spatial detection of neovascularization and other wet AMD signalling changes over time. Spectral-domain Optical Coherence Tomography (SD-OCT) can generate in-vivo cross-sectional visualisation of the retina and choroid layer, providing in-depth quantification of time-dependent parameters that have predictive value.
The predictive utility of SD-OCT has been proven in a longitudinal study on 330 AMD eyes in 244 patients, over five years [2]. Algorithms use the patient-derived data to generate a risk score. Being able to predict up to eleven months before discerned progression, investigators have found a formula to successfully quantify AMD associated imaging biomarkers and stratify patients with likelihood of developing wet AMD.
Dynamika, IAG’s imaging data platform, is utilised in clinical development where quantitative imaging biomarkers are pivotal. AMD trials benefit from efficient data management, early efficacy endpoints and increased trial performance transparency.
[1] Pennington K L, DeAngelis M M (2016) “Epidemiology of age-related macular degeneration (AMD): associations with cardiovascular disease phenotypes and lipid factors” Eye and Vision.
[2] Sisternes L, Simon N, Tibshirani R, Leng T, Rubin D L (2014): “Quantitative SDOCT Imaging Biomarkers as Indicators of Age-Related Macular Degeneration Progression” Investigative Ophthalmology and Visual Science Vol. 55 [7093-7103].
Experience: Imaging
- Colour Fundus Photography (CFP)
- Fundus Autofluorescence (FAF)
- Spectral-domain Optical Coherence Tomography (SD-OCT)
Publications
Since 2007, over 2000 articles were published to cover scientific discoveries, technology break-throughs and special cases. We list here some critically important papers and abstracts.
Testimonials
Combining our technologies and business advisory services with promising life science companies has yielded spectacular results over the past five years. As a trusted partner to many biotech and pharma companies, IAG’s team is proud to share your words and quotes.

